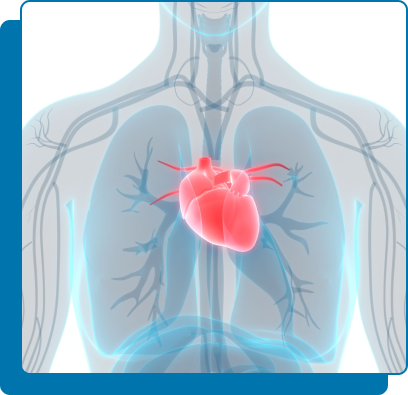
Aorta is the largest artery of the body. The average diameter in the chest (thoracic aorta) is up to 28 mm, and around 20 mm in the abdomen (abdominal aorta). The normal diameter of the abdominal aorta can range between 14 – 30 mm.
When the abdominal aorta develops a weakness and bulges or expands in size more than 1.5 times its average normal diameter, it is called an aortic aneurysm. The pressure of the blood with every heart beat can cause further weakening of the aorta, causing it to bulge (much like a balloon).
The term aortic aneurysm is used interchangeably with the term aortoiliac aneurysm, because the iliac arteries are quite often also aneurysmal in the presence of an abdominal aortic aneurysm and their treatment strategy is typically similar.
Isolated iliac artery aneurysms are rare. A common iliac artery is considered normal if its diameter is less than 17mm (males) or 15mm (females), ectatic if between 17-25mm, and aneurysmal if above 25mm.
if they affect the abdominal aorta proximally to the origins of the renal arteries; these are one of the types of thoracoabdominal aneurysms. An aneurysm that involves the renal arteries may be classified as juxtarenal or pararenal.
Infrarenal aneurysms
if they affect only the segment of the aorta distally to the origins of the renal arteries; these are the most common type (about 95%)
If the aneurysm is not treated, the aortic wall continues to weaken and the aneurysm to enlarge. Eventually, the aneurysm becomes large enough and its wall too weak and bursts (ruptures). A ruptured aneurysm can cause very severe internal bleeding leading to shock and death in most cases.


Feeling of pulsations in your abdomen, similar to a heartbeat
Pain in the abdomen or in the lower back. If there is severe pain of sudden onset, it is likely that the aneurysm is about to rupture. A less common type of aneurysm, the inflammatory aortic aneurysm, which is characterised by retroperitoneal fibrosis and obstruction of the ureters, is more likely to cause pain
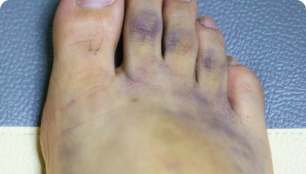
In rare cases, your feet and toes may develop areas with bluish discolouration and pain, because of embolization (ie shedding of debris downstream) from the the aneurysm. Another term for peripheral atheroembolism is “blue toe syndrome
Aortic aneurysms are commoner in men. You are at increased risk of developing an aortic aneurysms if you are:
- A man over 60 years of age. The risk increases with the age. Among men of 65-80, the percentage of those with an AAA is 2-5%. Among women of the same age, the percenage is up to 1%
- A smoker
- A man whose father or brother has/had got an aneurysm
- A man with either coronary or peripheral arterial disease
Your vascular surgeon will always attempt to save your limbs, with the latest technology available. At times, limb salvage may not be feasible despite the best efforts. In such situations, you may be recommended this operation for one of the following reasons:
The blood supply to your foot may have deteriorated, because the arteries of the leg have become narrowed or blocked. You may have developed severe pain in your foot waking you at night or even ulcers and black areas in the toes, foot or lower leg. After evaluation, if it is seen that the blood circulation cannot be improved to a sufficient enough stage to salvage the limb ( for example, in case of extensive gangrene or ascending infection), an amputation becomes necessary.
If you are diabetic or suffer from chronic renal failure, you may be prone to developing infections in the toes, foot which may extend to the lower leg. This condition may lead to sepsis which can threaten your life. In situations where these infections do npt respond to antibiotics , an amputation becomes necessary.
You will usually be admitted to the hospital one or two days before surgery so that there is enough time for the necessary investigations (blood tests, chest x-ray, electrocardiography, echocardiography etc) to be done. Your physician will generally require that 2 units of blood are available for you.
You may need to discontinue any anticoagulant, like Warfarin or Sintrom, or antiplatelet drugs like Clopidogrel (Iscover, Plavix) or Aspirin, for a few days, (if you have been prescribed these before) in order to reduce the risk for bleeding during the operation.
When you are admitted, your medical history will be recorded. Later, your vascular surgeon and the anaesthetist will visit you to explain the procedural details and clarify any doubts you may have. You will need to sign a consent document attesting to your understanding of the necessity for and risks associated with the operation.
The first part of any operation is the administration of anaesthesia. Your operation will be performed either under general anaesthesia or under regional anaesthesia (insertion of an epidural catheter in your back to provide pain relief during and after the operation). A urinary catheter will be placed in your bladder to monitor your urine output.
The amputation involves meticulously dividing the skin, fascia and muscles around the bones, at a healthy level. This is followed by dividing and tying the blood vessels and dividing the nerves, which is then followed by cutting of the bone(s) at an appropriate level to allow skin and muscle to cover the bone with stitches.
The amputation stump will be closed with either Nylon stitches or metal clips and will be bandaged. The sutures will usually be removed 15-20 days after the operation.
Following the operation you will return to your normal ward and you will be given all your fluids by a drip until you are able to eat and drink. The nursing and medical staff will administer pain medications to try to keep you free of pain. It is common to experience pain that feels to be a part of the leg that has been removed (phantom limb pain), but this can be helped with medication and rapidly disappears.
The various catheters will gradually be removed and you will become more mobile until you are fit enough to go home. You will be visited by the physiotherapist who will help you with your mobility, and even with your breathing (if you are thought a high risk for chest infection).
You will be instructed in bed exercises at first, and later urged to go from your bed to a chair. The physical therapist will have you begin walking with assistance as your wound heals, and you’ll learn how to use a wheelchair. As your rehabilitation progresses, an appointment will be made at the limb fitting centre to start you walking on a temporary artificial limb (“prosthesis”) and eventually you will have an artificial limb tailored to your needs.
Some alterations may be necessary at your home, especially in the bathroom and the stairs, before you are discharged. Following discharge, you will need to continue physiotherapy to encourage mobility with your artificial limb or wheelchair. You will usually be able to walk again (depending on the level of amputation), provided you have the motivation and fitness to do so.
Driving after amputation could be conceivable, either in an automated vehicle or with certain adaptations, but the hazards must be considered. Bathing may definitely require some assistance at first. To properly enter and exit the bathtub, you might additionally require grips or a hoist.
As with any operation there is a small risk of a heart attack or stroke or even of dying.
Chest infections can occur following this type of surgery, particularly in smokers, and may require treatment with antibiotics and physiotherapy.
At times, it is necessary to perform another amputation higher up in the leg if the wound does not heal. This may happen because of the relatively poor blood supply at the level of the amputation.
If the wound becomes infected, antibiotic treatment will be given, while occasionally, a new operation may be required.
If you experience symptoms of phantom limb, as mentioned above, appropriate medication can be prescribed to alleviate your symptoms.
Studies have found that amputees who engage in regular physical exercise feel better about themselves than those who are more sedentary.
Also, people who recover from an amputation are more likely to have greater job satisfaction, possibly because of changes in their attitudes regarding life goals
- You can learn how to adapt to having an artificial limb, including getting regular exercise, with the help of physiotherapy
- Do not put on weight, because ambulation with the artificial limb will be more difficult
- Quit smoking completely. If you continue, you are at an increased risk of a heart attack, stroke or of losing your remaining leg.
- Eat high fibre diet (plenty of fruit and vegetables) to prevent constipation
- Control your blood pressure, blood cholesterol and diabetes. Be punctual with your medication.
